|
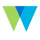
One of our central premises is that readiness is applicable to multiple settings and multiple innovations. The Robert Wood Johnson Foundation has generously funded research into how readiness can be measured, built, and used in decision-making process across FOUR distinct projects, bound together by a common thread of enhancing the tangible application of readiness. Readiness-focused technical assistance (RTA) model With CDC’s Office on Smoking and Health/Program Services Branch (OSH-PSB) With CDC-OSH, we are piloting readiness-focused technical assistance (RTA). RTA includes a readiness assessment, determining strategies to build readiness, and developing a readiness-building action plan. Our team provides regular support to project officers, who themselves are supporting ten different states/territories building readiness for state-specific tobacco prevention initiatives. As of November, most states completed their readiness assessment for their selected initiative. Using the assessment, OSH staff will be creating readiness-building action plans for each state/territory. They will then monitor progress on the action plans. Our team will provide ongoing support via weekly planning calls with key stakeholders at OSH, biweekly “office hours” for OSH staff to ask questions, and monitoring of a dedicated email account for inquiries. We are building toward a repository of policy-specific change strategies developed with OSH. This project will provide information about the implementation and effectiveness of RTA for building readiness. Readiness for Comprehensive Medication Management (CMM) in Healthcare Specialty Clinics: With Center for Medication Optimization Group, University of North Carolina Eshelman School of Pharmacy Medication misuse and abuse has a tremendous impact on healthcare costs ($528 billion annually spent on addressing medication misuse vs $450 billion spent on prescriptions). Pharmacy practice has recently embraced implementation science as one solution to accelerate the pace of healthcare change, drive effectiveness of medication optimization interventions, and facilitate replication and scaling. We are applying a readiness lens in about five UNC Specialty Healthcare clinics that are implementing a pharmacy practice intervention, Comprehensive Medication Management (CMM). In quarter one, we focused on setting the stage for success by building motivation in clinics and creating the two orientation trainings for participating pharmacists and readiness team. Given the increasing interest in medication optimization interventions, findings from this project will make a significant contribution toward an evidence-based readiness approach as a necessary part of effective implementation. Fostering Improved Police-Community Relationships. With Serve and Connect The relationships between police (as first-responders) and marginalized communities can impact progress toward a Culture of Health. Yet, tensions between police and community threatens well-being in communities where trust is fractured and reduces access to resources necessary for promoting community safety. Productive partnerships between police, community organizations, and members of the community may be a valuable tool for promoting equity. There is mounting evidence about the importance of police-community collaboration for addressing the underlying social factors which contribute to issues threatening community safety. However, few guidelines exist for fostering effective collaboration. We are refining a model for effective police-community collaboration which seeks to understand the factors that may facilitate or inhibit quality partnerships. Together with Relational Coordination Analytics @ Brandeis University and a community in Columbia, SC , we are using a joint readiness/ relationships model that seeks to support police and community partners in working together to improve community outcomes, particularly with black adolescents. This process can serve as a model that helps empower often-polarized groups to work together on shared goals of community safety, resilience and well-being. Readiness to Partner Cross-Sectorally for State-wide Behavioral Healthcare Integration
With the Farley Health Policy Center (FHPC) Integrated care is a patient-centered approach to addressing patient-population mental and physical health needs involving collaboration among mental health and primary care services and providers within a healthcare delivery system. Legislative changes in healthcare and growing emphasis on care coordination have catalyzed efforts to move toward integrated care. These efforts align with broader healthcare system goals of improving healthcare quality, health equity, utilization efficiency, and patient outcomes. At the state-level, cross-sector partnerships are a central strategy for improving care coordination and population level mental health outcomes. Defined as a formal alliance between two or more organizations representing different sectors of society (e.g., government, business, non-profit, philanthropy), cross-sector partnerships are particularly essential to addressing deep-rooted, complex community health issues. While the value of inter-organizational partnerships is recognized, the objective of establishing, developing, and sustaining cross-sector partnerships for statewide behavioral health coordination is highly challenging. A critical element to implementation success is the readiness of organizations to partner cross-sectorally. We aim to assess readiness for cross-sector partnerships to support the redesign and implementation of a continuum of community-based mental health services in Colorado. Future Directions Together, these project are developing innovative processes that can help funders and stakeholders be more effective and efficient with resources. Although an organization or state may not be ready to implement at the time of initial assessment, through the provision of readiness tools and TA, they may be able to become ready. This would ensure that resources can be equitably distributed to organization that may not often qualify for external funding, or otherwise have little experience with quality implementation. A focus on readiness can provide a mechanism for making a Culture of Health accessible to all.
3 Comments
1/29/2023 09:43:04 am
Reply
Leave a Reply. |
Categories
All
Archives
September 2023
|
 RSS Feed
RSS Feed
